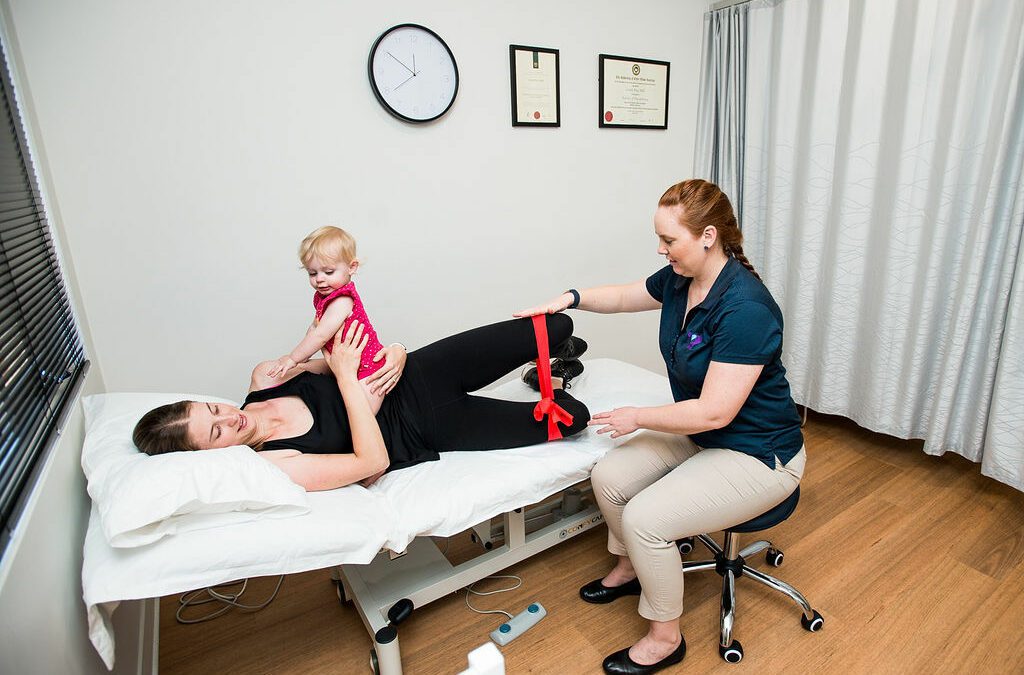
When you think about pelvic floor muscle exercises you generally think about strengthening but what about those who are not weak, but overactive.
There is a significant portion of the population who actually have an overactive pelvic floor.
People with an overactive pelvic floor often:
- Are easily stressed and hold ‘tension’ in their pelvic floor (similar to those who hold tension in their neck and shoulders).
- Are or have been super fit and their general muscle tone is high.
- Have a history of pelvic trauma including childbirth or significant gynaecological investigation or sexual violation or abuse.
How do you know if you have an overactive pelvic floor? Clinically, people with an overactive pelvic floor often report:
- that they try to do pelvic floor exercises, but ‘don’t really know if they are doing them correctly’.
- On command are able to contract their pelvic floor but are unable to relax it or are only able to relax it a little bit
- Painful intercourse (dyspareunia), either on penetration or deep inside
- Other pelvic pain
Why is this a problem?
An overactive pelvic floor is as unhelpful as a weak one. Initially, an overactive pelvic floor will often be identified following reports of pelvic pain or pain with intercourse. Over time, people with an overactive pelvic floor will often start to report symptoms of prolapse or incontinence. This is often associated with the muscles being fatigued and therefore not helpful when they are really needed eg. With a sneeze or a cough.
How do you get this checked?
If an overactive pelvic floor is suspected, you should always be provided management strategies prior to assessing for this. Giving you strategies to begin to manage the overactivity makes the assessment much easier for both the client and therapist and results in a more effective assessment.
The only way to assess for an overactive pelvic floor is via a vaginal examination (an ultrasound assessment cannot determine an over or underactive pelvic floor). This can be completed by a C&WH Physiotherapist. The aim of this assessment is to determine if and through what muscles the pelvic floor is overactive. The C&WH Physiotherapist will then give you management techniques to assist in ‘down-training’ your pelvic floor.
How do you ‘down-train’ your pelvic floor?
At Embodied Confidence, treatment will always start by assessing your breathing pattern. Often for people with an overactive pelvic floor, they use an apical breathing pattern (or chest breathing), rather than diaphragmatic breathing. Retraining diaphragmatic breathing alone can be enough to start to release the pelvic floor muscles. Following successful diaphragmatic breathing, during the vaginal examination a manual release may be completed to further down-train the muscles. Often the combination of breathing and manual release is enough to release these muscles and allow the client to progress to self management. If further treatment is needed, dilator therapy is also an option and this can be discussed with your C&WH Physio as needed.
Other strategies for managing pelvic pain:
- Use pain medication as needed for period pain or other cyclical pain– it’s really important for the brain to have as few experiences of pelvic pain as possible
- Consider positioning for intercourse – try different positions and try allowing the woman to be in control of the speed and depth to manage any pain experiences.
- Use a good quality lubricant during intercourse to reduce friction. Speak to your C&WH Physiotherapist regarding recommendations if you do not have one.
- In some instances, it will be recommended that you cease intercourse for a period of time if this is your main concern. Obviously, this is personal preference and for discussion between the client and their partner
- Involve your partner in appointments and discussions regarding managing pelvic pain, particularly regarding pain with intercourse. This allows both of you to receive the education available and make decision regarding how to progress with this concern as a couple
- If you are breastfeeding or menopausal, consider speaking to your GP regarding the option of using Vaginal Oestrogen. This is a topical oestrogen (only affecting the vaginal tissues) that helps support the tissues and compensate for the reduction of systemic oestrogen.
For further information, call Leonie at Embodied Confidence on 9143 1510 or book online